Lung cancer screening rates are low. This team is changing that.
Lung cancer remains the leading cause of cancer deaths in the United States, yet less than 6% of eligible individuals nationwide receive screening. This pales in comparison to breast cancer and colorectal cancer, which each boast screening rates upwards of 70%. This disparity is even more pronounced in rural areas like northern New England, where barriers to access surrounding lung cancer create significant obstacles to screening.
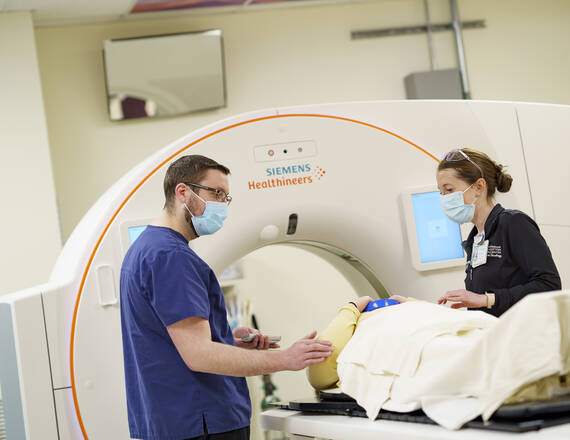
To help fix that problem, a team at Dartmouth Health and the Geisel School of Medicine at Dartmouth has worked to destigmatize the process and increase lung cancer screening rates for rural communities in New Hampshire and Vermont.
The initiative, which was conducted over a one-year period, has already had a substantial impact. The team’s interventions created a patient communications strategy and provider toolkit to increase awareness, improve eligibility identification, and support patient management.
The initiative was co-led by Karen Schifferdecker, PhD, MPH, a medical anthropologist and associate professor at The Dartmouth Institute for Health Policy & Clinical Practice, and Rian Hasson, MD, MPH, a thoracic surgeon, adjunct assistant professor of The Dartmouth Institute, and adjunct assistant professor of surgery at Geisel School of Medicine. By addressing barriers at multiple levels, they have increased the chances that patients will talk to their doctors about lung cancer screening. Now, providers are better equipped with resources and training on lung cancer screening guidelines, shared decision-making, and tobacco cessation counseling. Through thoughtful rebranding and inclusive messaging, the team has worked to shift perceptions and empower patients to take an active role in their lung health.
The team’s work was made possible by The Susan & Richard Levy Health Care Delivery Incubator, a joint venture between The Dartmouth Institute and Dartmouth Health. By funding innovative health care delivery solutions, the Incubator has enabled researchers to think creatively, recognizing that even seemingly small changes can have an outsized impact—which is exactly what the lung cancer screening project set out to accomplish.
Overcoming Barriers to Screening Through Human-Centered Design
More than 80% of cases of lung cancer, if detected early, are curable. Unfortunately, most people who are eligible and entitled to an annual lung screening computed tomography (CT) scan do not get tested.
“For many patients, when we find lung cancer, their cancer is advanced to the point of not being curable,” says Elliot Backer, MD, an interventional pulmonologist at Dartmouth Hitchcock Medical Center (DHMC) and assistant professor of medicine at Geisel School of Medicine. “So what we want to do is identify patients who are higher risk for the development of lung cancer and find those cancers earlier.”
As a result, the team sought to ascertain the biggest barriers preventing people from getting screened. Upon conducting stakeholder interviews, they quickly realized individuals who use tobacco products also tend to be less educated, have fewer resources, and may have less access to the healthcare system.
These factors, combined with a lack of public awareness and the stigma surrounding lung cancer’s association with smoking, contribute to low screening rates. Armed with these insights, the team developed a suite of interventions designed to empower patients, support providers, and streamline the screening process. An important first step was renaming the “Pulmonary Nodule Clinic” to the “Lung Health and Pulmonary Nodule Clinic”—a simple yet effective change that made it less intimidating for patients.
The team also created an educational patient brochure featuring inclusive and non-stigmatizing imagery and language, such as referring to “lung health” instead of “lung cancer.” The brochure invites patients to document their smoking history and determine their screening eligibility, making it easier to initiate conversations with healthcare providers.
The team says this friendly approach helps take the sense of blame off the individual and focuses on understanding nicotine addiction. By reframing website messaging and involving a patient advisor who survived lung cancer due to early screening, the brochure both resonated with the target audience and was user-friendly; it included a tear-off portion for patients to fill out and give to their providers to document their smoking history and eligibility for lung cancer screening.
Supporting Providers and Streamlining Systems
To support providers, one of the most impactful changes the team made was within Epic, the electronic health record (EHR) used by most healthcare systems across the country. The team noticed that there was no mechanistic way to keep track of a patient’s full history of smoking. If a provider entered new information, they also might lose prior information necessary to calculate “pack years” (how much a person smoked, for how long) and how long it has been since they quit.
Without an EHR field to efficiently calculate “pack years,” or to alert providers if information is missing, no mechanism for identifying patients eligible for screening exists. “Having the right EHR information and a way to alert providers about eligibility for screening or missing information to assess eligibility—that's a very scalable solution,” Schifferdecker says. Given that only 6% of eligible individuals currently get screened, scaling this Epic customization outside of DHMC, she adds, would likely have an incredible impact on increasing screening rates across the country, empowering clinicians to quickly identify patients who could benefit.
“The [team's] tool has definitely prompted providers and pulmonologists to order screening in a timelier manner for some patients who qualify,” said David Feller-Kopman, MD, section chief of pulmonary and critical care medicine at DHMC. “Especially with a more remote smoking history, like those who quit 7 to 10 years ago. It’s a great nudge.”
Driving Screenings Through Awareness
Beyond these initiatives, the team also drove patient engagement through creative marketing efforts. They updated the Dartmouth Health website with clear information on lung cancer screening, including patient testimonials to inspire others to take action. Website analytics showed a significant increase in traffic to these relevant pages, indicating growing interest and awareness among the community.
By addressing rural residents’ unique challenges, this team has enabled patients to be more informed and seek the right care for themselves. The team’s approach was designed so it could be replicated in rural areas across the country, serving as a model for improving preventive care access in underserved areas.
To learn more about The Susan & Richard Levy Health Care Delivery Incubator, please contact Bethany Solomon at 603-646-5134 or at Bethany.Solomon@hitchcock.org.